Occupational Therapy Can Help You Feel Better and Stay Active
June 16, 2021
Lymphedema is a chronic, lymphatic disease that causes swelling in parts of the body. The edema, or swelling, is a result of damage to the lymphatic drainage system. While there is no cure, it can be successfully managed with treatment so patients can feel better and stay active. There are two types – primary lymphedema, which can be hereditary and is often seen in the lower extremities, or secondary lymphedema, which can happen after surgery, radiation, physical trauma or infection. It is not uncommon for breast cancer patients to often experience secondary lymphedema if their lymph nodes are removed from their armpit area.
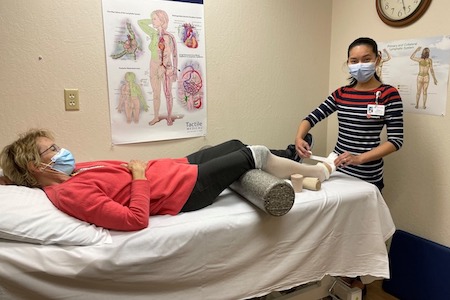
Tifanee Lin, OTR/L, CLT-LANA, is an Occupational Therapist (OT) and Certified Lymphedema Therapist (CLT) at Northern Nevada Medical Center in the Rehab and Sports Medicine Department. She has been an OT for almost 10 years.
How an OT Helps the Patient
Occupational therapists provide patients with the gold standard of treatment for lymphedema, known as complete decongestive therapy (CDT). This plan of therapy has two phases, intensive and long-term maintenance. “CDT involves techniques that decrease the swelling and help the area return to normal size, along with keeping the skin healthy,” says Lin. “One of the first things we do is manual lymph drainage.” She explains it is a form of light massage that helps stretch the skin to move lymphatic fluid out of the affected area. As a CLT, Lin teaches her patients diaphragmatic breathing, which helps open the deeper lymphatic pathways and increases movement of fluid. Phase II is the maintenance phase, which helps keep the body from building up tissue fluid.
Depending on the severity of the patient's lymphedema, they sometimes need the intensive phase of CDT in the clinic with Lin for four to five times a week, for more than four weeks. She explains that part of the therapy involves providing the patient and family training on self-manual lymphatic drainage, self-bandaging and home exercise recommendations, as well as skin and nail care education. “We also provide them with recommendations on compression garments to use for when they enter the long-term independent management of their lymphedema,” she says. “I fit them for compression garments that are appropriate for them. We also demonstrate the best techniques for putting their compression garments on and removing them, as some patients need adaptive equipment to do that.” Lin says since caregivers play an important role in patient success, it is crucial to make sure they are properly trained as well.
Lin emphasizes that education is extremely important for patients who have lymphedema or may be at risk for it. “Teaching patients to recognize the signs and symptoms of lymphedema and to examine themselves in a mirror, looking for changes is important. They should reach out to their healthcare provider if suspicious symptoms last longer than three months after surgery or appear anytime during or after radiation treatment,” she says. “Also, if you or a family member has been newly diagnosed with cancer and will need lymph nodes removed, ask your oncologist for a referral to a CLT. They can educate you on risk-reduction practices to help prevent lymphedema.”
